Stem cell therapy represents a rapidly advancing frontier in regenerative medicine, offering potential treatments for orthopedic conditions, autoimmune diseases, neurological disorders, and more. However, the proliferation of unproven therapies and unregulated clinics makes choosing the right medical professional a critical decision for patient safety and treatment efficacy.
Chronic pain from arthritis, sports injuries, or degenerative conditions drives millions of Americans to explore stem cell therapy each year, but the rapidly expanding field includes both legitimate medical practitioners and unregulated clinics making dangerous claims. The proliferation of unproven therapies has led to documented cases of blindness, tumor formation, and permanent neurological damage from treatments administered by unqualified providers. Choosing stem cell doctor qualifications requires systematic evaluation of credentials, experience, ethical practices, and regulatory compliance, not reliance on marketing promises or patient testimonials alone.
This guide outlines the essential doctor credentials regenerative medicine practitioners should hold, stem cell therapy red flags to avoid, critical patient questions for doctors during consultations, and the steps necessary to ensure quality of care while evaluating this promising but complex treatment option.
Key Takeaways
- Verify ABMS/AOA board certification plus specialized regenerative medicine training (ABRM, AASCP, IOF)
- Avoid clinics making miracle cure claims, using pressure tactics, or lacking peer-reviewed evidence
- Ask specific questions about cell sourcing, FDA compliance, procedure volume, and success rates
- Understand insurance reality: only FDA-approved HSCT for blood cancers is covered; orthopedic applications are out-of-pocket
- Prepare thoroughly with realistic 3-6 month outcome timelines and pre-procedure lifestyle modifications
What Is Stem Cell Therapy And Why Is It Important?
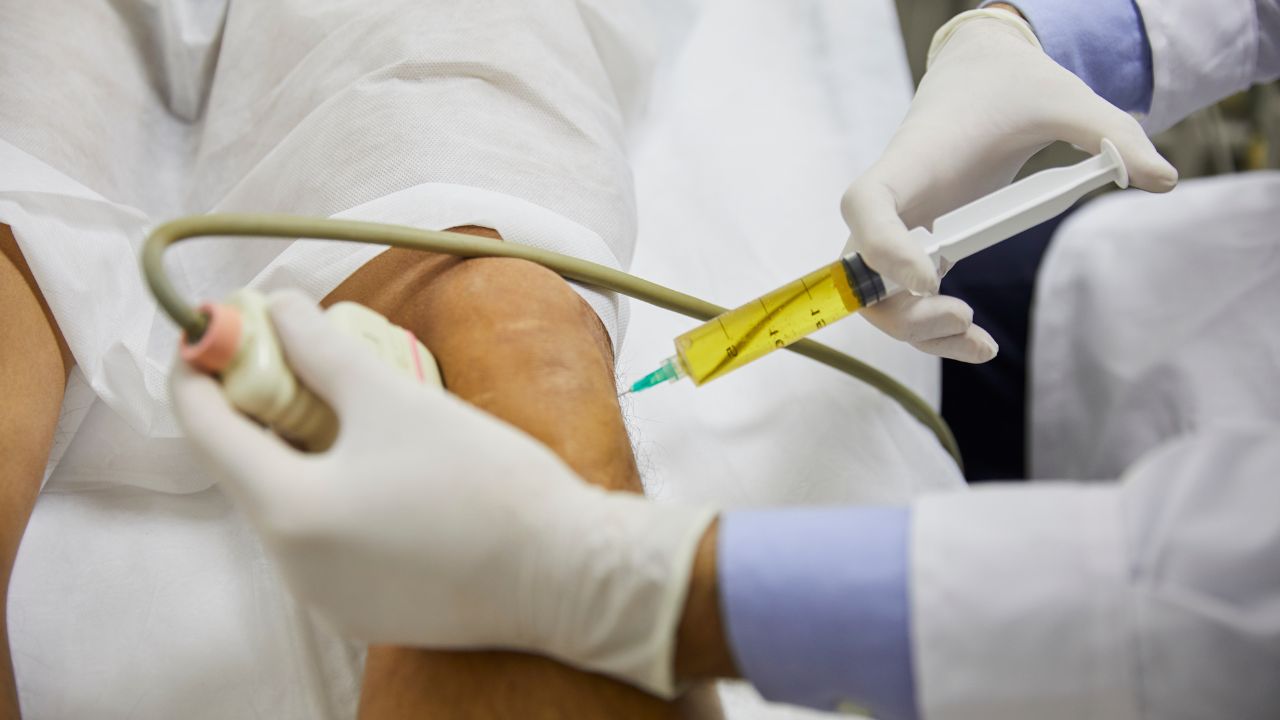
Stem cell therapy harnesses the body’s natural repair mechanisms to regenerate damaged tissue. The approach uses either your own cells (autologous) or donor cells (allogeneic) to treat conditions ranging from joint pain and degeneration to blood cancers. Orthopedic applications, such as knee arthritis, rotator cuff tears, and spinal disc injuries, rely on bone marrow aspirate concentrate (BMAC) or platelet-rich plasma (PRP) to stimulate healing without surgery.
Hematopoietic stem cell transplants for leukemia and lymphoma represent the only FDA-approved stem cell treatments for systemic disease. For a comprehensive overview of treatable conditions, see our guide on what conditions stem cell therapy can treat.
Conditions Treated by Stem Cell Therapy
| Condition Category | Treatment Approach |
| Orthopedic (knee/hip/shoulder pain, arthritis) | Autologous bone marrow aspirate (BMAC), PRP injections |
| Spinal (herniated discs, sciatica, back/neck pain) | Interventional spine medicine injections |
| Blood Cancers (leukemia, lymphoma) | FDA-approved hematopoietic stem cell transplants |
| Neurological (MS, neuropathy, spinal cord injuries) | Investigational protocols (clinical trials only) |
| Pain Management (fibromyalgia, migraines, CRPS) | Stem cell-derived growth factors, PRP |
Why Qualified Practitioners Matter: The FDA has documented severe adverse events from unproven therapies: blindness from intraocular injections, tumor formation, systemic infections, and permanent neurological damage. Choosing a properly trained physician is the only defense against these risks.
What Qualifications Should A Stem Cell Therapy Doctor Have?
No single “stem cell board certification” exists from traditional medical boards. Qualified practitioners hold primary board certifications in relevant specialties, orthopedics, pain management, physical medicine and rehabilitation (PM&R), or hematology/oncology, and pursue additional specialized training in regenerative medicine.
Medical Specializations to Look For:
- Orthopedics & Sports Medicine (joint/musculoskeletal issues)
- Pain Management (chronic pain, spinal interventions)
- Physical Medicine & Rehabilitation (PM&R)
- Hematology/Oncology (blood cancers requiring transplants)
Essential Certifications:
- ABMS/AOA Board Certification (primary specialty); verify via ABMS “Is My Doctor Certified?” tool
- American Board of Regenerative Medicine (ABRM); requires board certification + 1 year experience + 10% practice dedication + 20+ procedure case log
- American Academy of Stem Cell Physicians (AASCP); Fellowship/Diplomate certifications
- Interventional Orthobiologics Foundation (IOF); hands-on training in image-guided techniques
- Active State Medical License; verify via State Medical Board website
- Clean Disciplinary Record; check State Medical Board / National Practitioner Data Bank (NPDB)
Show Image Caption: A breakdown of the importance and prevalence of various credentials among qualified stem cell therapy practitioners.
Verification is mandatory. Never accept a doctor’s claims without independent confirmation through official licensing and certification databases.
What Are The Red Flags When Choosing A Stem Cell Therapy Doctor?
Unqualified practitioners exploit vulnerable patients using predictable tactics. Recognizing these patterns protects you from ineffective or dangerous treatments.
Signs of Improperly Trained Practitioners:
- No ABMS/AOA board certification in relevant specialty
- Lack of formal regenerative medicine training (ABRM, AASCP, IOF)
- No hospital privileges or institutional affiliation
- Unable to provide procedure volume statistics for your specific condition
- Practice run by non-physicians (physician assistants or nurse practitioners without MD/DO oversight)
Warning Signs of Scams:
- Miracle Cure Claims; “Single stem cell intervention treats autism, Alzheimer’s, and osteoarthritis simultaneously”
- No Peer-Reviewed Evidence; relying solely on testimonials rather than published clinical data
- Pressure Sales Tactics; demanding substantial upfront payments ($10,000+), high-pressure seminars, “limited-time offers”
- FDA Non-Compliance; falsely equating FDA facility registration with FDA treatment approval; claiming “minimally manipulated” for heavily processed cells
- No Informed Consent; failing to provide comprehensive written documentation of risks, benefits, and alternatives
- Testimonial-Only Marketing; no objective success rate metrics or peer-reviewed study citations
Show Image Caption: Analysis of red flag indicators, showing their frequency in rogue clinics and their impact on patient risk.
Case Study: Patient B sought macular degeneration treatment at an online-promoted clinic. The physician lacked ophthalmology training and injected adipose-derived stem cells into the patient’s eyes without FDA oversight or Institutional Review Board (IRB) approval. The result: permanent blindness in both eyes, a documented adverse event highlighted in FDA safety warnings.
What Questions Should You Ask Your Stem Cell Therapy Doctor?
A thorough consultation is your best protection against unethical practices. These patient questions for doctors evaluate both the physician’s qualifications and the proposed treatment’s legitimacy.
Doctor’s Approach to Patient Care:
- “Are you board-certified by ABMS or AOA, and in what specialty?”
- “What specific, formal training do you have in regenerative medicine (ABRM, AASCP, IOF)?”
- “How many times have you performed this exact procedure for my specific condition?”
- “What is the source of stem cells, autologous (from my body) or allogeneic (from a donor)?”
- “If using donor cells, what is the screening process for infectious diseases and genetic abnormalities?”
- “Is this treatment FDA-approved for my condition, or is it part of an FDA-authorized Investigational New Drug (IND) clinical trial?”
- “What are the objective success rates, and can you provide peer-reviewed studies supporting these numbers?”
- “What is the total cost, and what does it include?”
- “What is your protocol if an adverse reaction occurs, and who handles emergency care?”
Risks & Side Effects to Ask About:
- Infection risk at injection site or systemically
- Immune rejection (for allogeneic/donor cells)
- Tumor formation potential from uncontrolled cell growth
- Procedure-specific complications (nerve damage, tissue scarring)
- Long-term safety data gaps (many therapies lack 10+ year follow-up studies)
Success Rates by Condition
| Condition Type | Success Rate Range | Key Factor |
| Orthopedic (joint/MSK) | 65-85% | Physician experience, cell quality |
| Autoimmune/Inflammatory | 45-78% | Protocol precision, patient selection |
| Neurological | 32-65% | Highly variable, experimental status |
| Blood Cancers (HSCT) | 55-72% | Donor matching, disease stage |
Source: DVC Stem, ISSCR Guidelines, peer-reviewed literature synthesis
Show Image Caption: Correlation between doctor experience levels, treatment success rates across different conditions, and overall patient satisfaction.
Alternative Treatments: Always ask about less invasive or FDA-approved options: physical therapy, traditional surgery (joint replacement), PRP injections alone, radiofrequency ablation, spinal cord stimulation, or conservative pain management solutions. A legitimate doctor discusses alternatives and helps you understand why stem cell therapy is, or isn’t, the best choice for your specific case.
How Can You Evaluate A Stem Cell Therapy Doctor’s Experience?
Experience directly correlates with treatment outcomes. Doctors performing 100+ procedures annually demonstrate mastery of injection techniques, patient selection criteria, and complication management that newer practitioners lack. Verify experience through specific metrics, not marketing claims.
Key Metrics:
- Procedure volume; minimum 20+ for ABRM certification; ideal 100+ for complex cases
- Years in regenerative medicine; 5-10+ years preferred for consistent outcome data
- Published case studies or peer-reviewed research; demonstrates clinical outcomes tracking
- Hospital privileges at accredited facilities; third-party credentialing verification
- Fellowship training; IOF, FDA, or ISSCR programs indicate advanced specialization
- Active clinical trial participation; involvement in formal research protocols
Assessing Patient Reviews:
- Verify across multiple platforms (Google, Healthgrades, Vitals, RateMDs)
- Look for specific outcome mentions; “pain reduction 70%,” “returned to tennis in 4 months”
- Check for transparency in risk discussion and informed consent process
- Note follow-up care quality and post-procedure support
- Red flags: multiple complaints about pressure tactics, surprise costs, or unavailable doctors post-treatment
- Prioritize recent reviews (last 1-2 years); older reviews may not reflect current practice standards
Success Example: Patient A consulted a board-certified orthopedic surgeon with an IOF fellowship and 8+ years of regenerative medicine experience. The treatment: bone marrow aspirate concentrate (BMAC) for grade III knee pain osteoarthritis via ultrasound-guided injection. Result: 75% pain reduction, returned to hiking and golf within 6 months, outcomes tracked in a formal clinical registry. The doctor provided transparent success rate data (68% of patients achieving ≥50% pain reduction) before treatment.
What Are The Ethical Concerns With Stem Cell Therapy?
Ethical stem cell practice requires informed consent, transparent sourcing, and regulatory compliance. Legitimate doctors operate under FDA oversight (21 CFR Part 1271), disclose all risks, including treatment failure, and acknowledge when therapies remain investigational.
Ethical Guidelines:
- Informed consent; comprehensive multi-page document detailing risks, benefits, alternatives, and realistic outcome expectations
- Ethical cell sourcing; transparent documentation of autologous harvest or FDA-screened donor cells
- FDA regulatory compliance; follows 21 CFR Part 1271 for cell processing; operates under IND (Investigational New Drug) for experimental therapies
- Transparency in cell processing; discloses manipulation methods, culture expansion, genetic modification
- Patient rights; clear protocols for treatment withdrawal, second opinions, and medical record access
- Scientific integrity; bases claims on peer-reviewed evidence or IRB-approved clinical trials only
Verifying Ethical Practices:
- Provides detailed cell source documentation (autologous harvest site and method, or FDA-screened donor registry)
- Uses multi-page informed consent with explicit risk/benefit/alternative discussion
- Operating under IND if investigational; strictly follows 21 CFR Part 1271 for minimal manipulation
- Cites peer-reviewed studies; acknowledges outcome variability and treatment limitations
- Transparent about complication rates with clear adverse event reporting protocols
Unethical Practice Red Flags:
- Vague about cell origin; mentions “offshore sourcing” or “international tissue banks”
- Rushed consent process (single-page form); minimizes risks or guarantees outcomes
- Claims FDA bypass via “autologous loopholes” or “minimal manipulation” for heavily processed cells
- Relies exclusively on video testimonials without objective outcome data
- No mention of adverse event risks or emergency protocols
What Should You Know About Clinical Trials And Stem Cell Therapy?
Clinical trials establish safety profiles, optimize protocols, and generate the evidence base required for FDA approval. Participation offers access to cutting-edge treatments with rigorous monitoring, but also carries investigational risks. Critical distinction: A ClinicalTrials.gov listing does NOT mean FDA approval, it simply confirms trial registration.
How Trials Impact Development:
- Optimize cell dosing, injection techniques, and treatment timing through systematic testing
- Establish objective success rates through randomized controlled studies
- Identify adverse events through mandatory systematic tracking and reporting
- FDA approval requires completed Phase I (safety), Phase II (efficacy), and Phase III (large-scale confirmation) trial data
- Validate new cell types (e.g., umbilical cord-derived MSCs) or delivery methods (e.g., intra-articular vs. intravenous)
Questions Before Participating:
- “What phase is this trial (I, II, III), and what does that mean for safety and efficacy data?”
- “What are the documented risks from earlier trial phases?”
- “What is the primary endpoint being measured, and what success rate has been observed so far?”
- “Will I receive a placebo, and what is the randomization ratio?”
- “What is the safety monitoring protocol for adverse events?”
- “Can I withdraw at any time without penalty or loss of alternative treatment options?”
- “Who is funding this trial, academic institution, pharmaceutical company, or the clinic itself?”
- “Has the protocol been IRB-approved, and can I see the approval documentation?”
Phase I trials focus on safety in small groups (10-30 patients). Phase II trials test efficacy in 50-200 patients. Phase III trials involve hundreds to thousands of patients to confirm results before FDA review. Earlier phases carry higher risk but may offer breakthrough treatments unavailable elsewhere.
How Much Does Stem Cell Therapy Cost And Is It Covered By Insurance?
Most regenerative stem cell therapies are NOT covered by insurance because they remain investigational or are classified as elective. Only FDA-approved hematopoietic stem cell transplants (HSCT) for blood cancers receive coverage. Patients pay out-of-pocket for orthopedic and pain management applications.
Typical Costs
| Treatment Type | Cost Range | Insurance Coverage |
| PRP Injection (single joint) | $500 – $2,500 | NOT covered |
| BMAC for Knee/Hip | $3,000 – $8,000 | NOT covered (except FDA trials) |
| Adipose-Derived Stem Cells | $5,000 – $15,000 | NOT covered |
| Spinal Disc Regeneration | $5,000 – $12,000 | NOT covered |
| HSCT for Blood Cancers | $100,000 – $300,000+ | COVERED (FDA-approved) |
| Sports Injury Treatment | $2,000 – $7,000 | NOT covered |
Insurance Coverage Reality:
- FDA-approved HSCT for blood cancers; covered by Medicare, Medicaid, and private insurance
- Investigational therapies; NOT covered unless patient enrolled in insurance company-sponsored clinical trial
- Regenerative orthopedic treatments; classified as experimental/elective; NOT covered
- Medicare Part B; explicitly does NOT cover stem cell therapy for arthritis, joint pain, or degenerative conditions
- HSAs/FSAs; may be used for qualified medical expenses if treatment is deemed medically necessary by primary care physician
Cost transparency is mandatory. Legitimate doctors provide itemized pricing before treatment, covering cell processing, facility fees, imaging guidance, and follow-up visits. Beware of clinics requiring full payment upfront or offering “package deals” for multiple unrelated conditions, these are pressure tactics designed to bypass informed decision-making.
How To Prepare For Stem Cell Therapy Treatment With Your Chosen Doctor?
Proper preparation maximizes treatment efficacy and minimizes complications. The preparation phase begins at your initial consultation and extends through procedure day, covering medical clearance, lifestyle modifications, and logistics planning.
Initial Consultation Discussion:
- Detailed treatment plan; cell harvesting method, processing facility location, injection technique and image guidance
- Expected outcomes and realistic timeline; most patients see results at 3-6 months, not immediately
- Preparation requirements; lab work (CBC, metabolic panel), imaging (X-ray, MRI), medication adjustments
- Cell source confirmation; autologous (from your bone marrow or adipose tissue) vs. allogeneic (screened donor)
- Post-procedure restrictions; activity limitations, physical therapy protocol, gradual return to exercise
- Follow-up schedule; outcome tracking visits at 6 weeks, 3 months, 6 months, and 12 months
Pre-Procedure Preparation:
- Understand the procedure; request written materials explaining each step; watch educational videos if available
- Review informed consent thoroughly; read every page; ask questions about any unclear language
- Complete medical clearance; labs (to rule out infection, anemia), imaging (baseline joint condition)
- Stop blood thinners and NSAIDs 1-2 weeks pre-procedure; aspirin, ibuprofen, naproxen impair healing
- Quit smoking 2 weeks before; nicotine impairs stem cell function and reduces treatment success rates by 30-40%
- Arrange transportation; required if sedation or anesthesia used during bone marrow harvest
- Plan recovery time off work; 1-3 days for most procedures; 1-2 weeks for physically demanding jobs
- Set realistic expectations; understand that results develop gradually over 3-6 months, not overnight
Patients who follow preparation protocols experience fewer complications and better outcomes. Non-compliance with pre-procedure instructions, particularly continuing NSAIDs or smoking, significantly reduces stem cell viability and treatment effectiveness.
Is Stem Cell Therapy Right For You?
Stem cell therapy offers legitimate treatment potential for select orthopedic, pain management, and hematologic conditions when delivered by qualified practitioners using evidence-based protocols. The decision requires careful evaluation of the doctor’s credentials, treatment appropriateness for your specific condition, and realistic outcome expectations that prioritize quality of care over marketing promises.
Key Decision Factors:
- Doctor qualifications; ABMS/AOA board certification + specialized training (ABRM, AASCP, IOF)
- Experience level; 5-10+ years in regenerative medicine, 100+ procedures for complex cases
- Ethical practices; transparent cell sourcing, comprehensive informed consent, strict FDA compliance
- Red flag absence; no miracle cure claims, no pressure tactics, no testimonial-only marketing
- Cost transparency; all-inclusive estimates provided upfront; realistic insurance coverage discussion
- Clinical evidence support; peer-reviewed studies or legitimate IRB-approved clinical trial participation
Action Steps:
- Verify credentials via ABMS “Is My Doctor Certified?” tool and state medical board website
- Request documentation; peer-reviewed studies supporting treatment, written treatment plan with risks/benefits
- Seek multiple opinions; consult 2-3 specialists plus your primary care doctor before committing
- Check reviews across platforms: Google, Healthgrades, Vitals, RateMDs (prioritize recent reviews)
- Confirm regulatory status; FDA-approved for your condition, or operating under a legitimate IND clinical trial
- Understand costs; request itemized all-inclusive estimates; clarify insurance coverage reality
- Prepare thoroughly; complete all medical evaluations, make required lifestyle modifications
- Monitor outcomes; document symptoms, attend all follow-up visits, report adverse events immediately
Final Guidance: Legitimate stem cell therapy requires patience, realistic expectations, and evidence-based medicine, not miracle cure promises. Systematically verify credentials, demand transparency, and refuse to be rushed into treatment decisions. The right doctor will welcome your questions, provide detailed documentation, and acknowledge both the promise and limitations of regenerative medicine.
Ready to explore regenerative medicine with a qualified specialist? Contact the Regenerative Institute of Newport Beach to schedule a consultation with Dr. Khyber Zaffarkhan, a board-certified expert in stem cell therapy and pain management.